MIGRAINE
Migraine, a condition that is often misunderstood as a simple headache but is, in reality, a chronic neurological disorder that can significantly disturb daily life, mental clarity, and emotional balance.Migraine is directly associated with the brain and nervous system. Along with intense headache, it may present with symptoms such as nausea, sensitivity to light and sound, irritability, fatigue, and reduced concentration. Because migraine affects neurological functioning, its management should not be limited to medication alone. Instead, it should involve holistic approaches that calm the nervous system and improve oxygen supply to the brain.

Before beginning any learning session or therapeutic discussion related to neurological health, it is essential to prepare the brain for better focus and absorption. One of the simplest yet most powerful techniques to achieve this is deep conscious breathing. Proper breathing increases oxygen availability, improves neural coordination, and enhances mental alertness. It also helps synchronize neuronal activity, allowing the brain to function more efficiently.
To achieve this state of calm alertness, we introduced a Box Breathing Technique, which is especially beneficial for conditions like migraine. This technique is widely used to stabilize brain activity, regulate stress hormones, and promote nervous system balance.
In box breathing, inhalation, retention, exhalation, and pause are all done for equal durations. The process begins with a slow and deep inhalation for a count of four. This is followed by holding the breath for four seconds, a phase known as Kumbhaka. After this, the breath is slowly exhaled for another count of four, allowing the lungs to release carbon dioxide efficiently. Finally, the breath is again held for four seconds before beginning the next cycle. This completes one round of box breathing.
Practicing this breathing pattern for three to five rounds helps maximize oxygen intake while efficiently removing carbon dioxide from the lungs. The brief breath retention enhances oxygen exchange at the cellular level and supports better circulation to the brain. As a result, the brain receives adequate oxygen and glucose, immediately improving focus, relaxation, and mental clarity.
Many participants may notice a sense of calmness, lightness in the head, and improved concentration after just a few rounds. This happens because controlled breathing activates the parasympathetic nervous system, which is responsible for relaxation and healing. It also reduces stress-related triggers that commonly worsen migraine episodes.
There is often a concern regarding breath retention, especially among individuals with blood pressure or heart-related issues. However, when practiced gently for a short duration of three to four seconds, box breathing is generally safe. In fact, short and controlled breath retention can help regulate blood pressure by calming the autonomic nervous system. Nevertheless, it should always be practiced comfortably, without strain.
This breathing practice is also highly beneficial for students and working professionals, as it supports better memory, concentration, and mental endurance. While there is no specific “memory gland,” improved oxygen supply and neural efficiency naturally enhance cognitive functions such as memory retention and recall.
Box breathing does not require any special time, posture, or environment. Although practicing it in the morning is ideal, it can be done at any time during the day. In today’s fast-paced lifestyle, even dedicating two to three minutes within 24 hours can bring noticeable changes over time. Like any natural therapy, consistency is key. The benefits deepen when the practice becomes a part of daily routine.
Breathing is the most fundamental function of life, yet it is often taken for granted. Conscious breathing helps cleanse the lungs, balance the nervous system, and nourish the brain. For migraine sufferers, this simple practice can become a powerful supportive tool in long-term management.
In conclusion, incorporating box breathing into daily life is an easy, time-efficient, and natural method to improve neurological health. It supports mental calmness, enhances concentration, and plays a supportive role in managing migraine. When practiced regularly, it becomes not just an exercise, but a lifelong habit for better health and awareness.
Migraine Management Through Box Breathing and Naturopathic Understanding
Regular practice of box breathing not only supports neurological balance but also significantly improves overall energy levels, freshness, coolness of the mind, and emotional calmness. When practiced daily for at least 10 consecutive days, noticeable changes begin to appear. By the 11th day, individuals often experience improved mental clarity, reduced stress, and enhanced emotional stability. This gradual transformation highlights the importance of consistency rather than expecting instant results.
Individuals suffering from anxiety, hyperactivity, restlessness, and emotional instability often observe visible changes in their behavior through regular breathing practice. Patience levels improve, reactions become calmer, and impulsive responses gradually reduce. In today’s fast-paced lifestyle, especially among the younger generation, impatience and mental agitation have become common concerns. Box breathing helps counter these tendencies by calming the nervous system and restoring inner balance.
This simple breathing technique, when practiced regularly, brings subtle yet powerful changes. Many people describe it as a “miracle practice” because of its wide-ranging benefits on mental, emotional, and neurological health. Conscious breathing is not an optional activity but a basic necessity for healthy living, as it supports every system of the body, particularly the brain and nervous system.
Introduction to Migraine
Now, let us move toward understanding migraine in detail. Most individuals are familiar with the term migraine, yet there is often confusion regarding its nature and severity. Migraine is not merely a headache; it is a chronic neurological condition that requires proper understanding and holistic management.
Headache is the most common symptom observed in migraine, but it is important not to confuse every headache with migraine. Many times, headache can occur due to temporary factors such as dehydration, disturbed sleep patterns, excessive screen exposure, mental stress, or aggravation of Pitta dosha. Such headaches may last for a short duration and resolve with simple lifestyle correction. Therefore, experiencing a headache does not necessarily indicate migraine.

However, headache remains a key symptom during migraine diagnosis. Migraine-related headaches are usually intense, recurring, and disturbing, and they significantly affect an individual’s daily routine. Whether at the workplace, during studies, household activities, or social interactions, persistent headache creates irritation and discomfort. The mind remains constantly focused on pain, making it difficult to divert attention toward productive tasks.
This continuous discomfort leads to reduced concentration, irritability, emotional imbalance, and decreased work efficiency. The severity of migraine pain often prevents immediate mental distraction, as the pinching or throbbing sensation dominates awareness. Over time, this can affect both professional performance and personal relationships.
Immediate and Preventive Aspects of Migraine
Migraine also presents certain immediate effects that require attention for prevention and control. Understanding early warning signs and triggers plays a crucial role in managing migraine episodes effectively. Naturopathy focuses on identifying these triggers and addressing them at the root level rather than merely suppressing symptoms.
Global Prevalence of Migraine
According to research conducted in the United States, approximately 39 million people suffer from migraine each year. On a global scale, the actual number is believed to be significantly higher, potentially three times more than reported. Studies indicate that nearly 70% of individuals experiencing recurrent headaches are diagnosed with migraine. This data highlights the widespread nature of migraine and the urgent need for effective, long-term management strategies.
Types of Migraine: Episodic and Chronic
Migraine is broadly classified into episodic migraine and chronic migraine. Understanding this classification is important from both a medical and naturopathic perspective. While the core treatment approach in naturopathy remains focused on root-cause correction, the classification helps in understanding the severity and progression of the condition.
Episodic migraine refers to migraine attacks occurring less than 14 times per month, on average. These attacks may vary in intensity and duration but do not occur daily. On the other hand, chronic migraine is diagnosed when migraine episodes occur more than 14 to 15 days per month, and in some cases, even on a daily basis.
Interestingly, the severity of suffering does not always correlate with frequency. Some individuals with chronic migraine may experience milder pain compared to those with episodic migraine, yet the constant presence of discomfort affects their quality of life. Migraine remains a complex and sometimes mysterious condition, requiring individualized and holistic management.
Naturopathic Approach to Migraine
From a naturopathic point of view, the goal is not merely to label migraine as episodic or chronic, but to identify the level of dosha imbalance, lifestyle disturbance, nutritional deficiency, and nervous system overload. Treatment focuses on detoxification, nervous system relaxation, dietary correction, hydration, breathing techniques, and stress management.
By integrating practices like box breathing along with naturopathic therapies, migraine can be managed effectively and sustainably. Addressing the root cause allows gradual healing, improved tolerance to triggers, and long-term relief.
Understanding Migraine: Causes, Triggers, and the Naturopathic Perspective
Migraine is a complex health condition that does not affect every individual in the same manner. Its occurrence, intensity, and frequency largely depend on several personal factors such as the individual’s symptoms, age, gender, lifestyle, and presence of other associated health issues. Therefore, the most important aspect in understanding migraine is taking a detailed history of the patient. Each case of migraine is unique, and management should always be personalized.
For academic and general understanding, migraine can be classified into different types based on certain criteria. However, before classification, it is essential to understand the root causes behind why people suffer from migraine.
Root Causes of Migraine
To date, modern medical science has not identified a single, definite cause of migraine. Despite years of extensive research conducted on large groups of people, no specific universal cause has been scientifically proven. What research does suggest, however, is that migraine results from a combination of multiple factors, and these factors differ from person to person.
Genetic Factors
One of the most common and widely accepted causes of migraine is genetics. Individuals who have a family history of migraine are more prone to develop this condition. When migraine runs in families across generations, the chances of experiencing migraine episodes increase significantly. This genetic predisposition makes certain individuals more sensitive to triggers compared to others.
Environmental Factors
Environmental conditions play a major role in triggering migraine episodes. Many people notice symptoms such as dizziness, imbalance, heaviness in the head, or headache when exposed to polluted environments, smoke, or areas with burning fumes. These pollutants enter the body through breathing, affect the lungs, and eventually impact brain functioning.
Temperature changes are another major environmental trigger. Extreme heat, excessive cold, or sudden fluctuations in temperature can provoke migraine attacks. It has been commonly observed that many migraine sufferers experience more frequent episodes during the summer season due to high temperatures. On the other hand, some individuals are sensitive to cold weather and experience increased migraine episodes during winter, especially in regions with extreme cold or snowfall. These reactions vary according to individual body constitution and tolerance levels.
Serotonin Imbalance
Serotonin is an important neurotransmitter that regulates mood, sleep, and neurological balance. Any imbalance in serotonin levels—whether excessive secretion or deficiency—can disturb neuronal activity in the brain. This imbalance can create pressure, stress, and altered pain perception, making it one of the contributing factors in migraine development.
Abnormal Electrical Activity in the Brain
The brain functions through continuous electrical activity within nerve cells. When this electrical activity becomes irregular or excessive, it can disrupt normal neurological signaling. Such disturbances may result in headaches, pain, or migraine attacks. Irregular electrical patterns are often linked with chronic or recurring migraines.
Migraine: Disease or Tendency?
It is important to understand that migraine is not exactly a disease in the strict sense. A disease usually refers to a condition where something is structurally or functionally damaged and requires medical repair. Migraine, however, is better described as a condition or a tendency.
A tendency or condition is generally reversible and can often be managed or improved through lifestyle modifications such as changes in diet, daily routine, sleep patterns, stress management, and avoidance of triggers. Migraine develops due to negligence, continuous exposure to stimulants, and repeated triggering factors rather than permanent damage to an organ.
Migraine is called a tendency because its intensity and duration vary greatly among individuals. Some people may experience headache for a few hours, while others may suffer for two days or even longer. The frequency and severity depend entirely on the individual’s internal balance and external environment.
Ayurvedic and Naturopathic Viewpoint
According to Ayurveda and naturopathy, migraine is closely linked to the imbalance or aggravation of Pitta dosha. The human body is governed by three doshas—Vata, Pitta, and Kapha. Among these, excess Pitta, which represents heat, metabolism, and intensity, plays a central role in migraine.
When Pitta becomes aggravated due to improper diet, irregular routine, stress, heat exposure, or emotional disturbances, it affects the nervous system and blood circulation in the brain, leading to migraine symptoms. Therefore, from an Ayurvedic and naturopathic perspective, balancing Pitta through diet, lifestyle, breathing techniques, and natural therapies is the key to managing migraine effectively.
Role of Pitta Aggravation and Dietary Stimulants in Migraine
When migraine occurs, it is not caused by the aggravation of Pitta alone. In most cases, migraine develops due to a combination of multiple internal and external factors. Although Pitta dosha plays a dominant role according to Ayurveda and naturopathy, several stimulants and triggers further aggravate the condition and intensify pain and headache episodes.
These stimulants act by increasing heat, irritation, and hypersensitivity in the nervous system, making migraine attacks more frequent and severe. Identifying and eliminating these triggers is a crucial part of migraine management.
Alcohol as a Major Migraine Trigger
Alcohol is one of the strongest stimulants known to aggravate migraine. From a naturopathic perspective, all forms of alcohol are strictly prohibited. Although some conventional studies suggest that small amounts of red wine may benefit heart health, the same red wine is a powerful migraine trigger.
Red wine, in particular, is well known for triggering migraine attacks due to its effect on blood vessels, neurotransmitters, and heat production in the body. For individuals prone to migraine, all types of alcohol—red wine, beer, spirits, or any other form—should be completely avoided, as they significantly increase the intensity and frequency of headache episodes.
Dairy Products and Processed Cheese
Dairy products, especially processed cheese, are another major dietary stimulant for migraine sufferers. Processed cheese contains high levels of sodium, unhealthy fats, and additives that can trigger inflammation and water retention. Additionally, many individuals suffer from lactose intolerance or mild dairy allergies, which further burden the digestive system.
Dairy products are heavy to digest, lack dietary fiber, and often slow down metabolism. Poor digestion leads to toxin accumulation, which indirectly affects brain function and aggravates migraine symptoms. Therefore, dairy products—particularly cheese and processed dairy—are commonly advised to be avoided from the very first day of migraine treatment in naturopathic practice.
Coffee and Caffeine Sensitivity
Coffee is one of the most common yet underestimated migraine triggers. Many people believe that coffee or tea provides temporary relaxation or relief from headache. However, caffeine directly stimulates the nervous system and can worsen migraine by making neurons hyperactive.
Caffeine interferes with normal neurological signaling and increases brain sensitivity. This effect is not limited to regular coffee alone. All forms of coffee, including green coffee, organic coffee, matcha coffee, or filtered coffee, have similar stimulating effects and should be avoided by migraine patients. Despite common misconceptions, the source or quality of coffee does not reduce its potential to trigger migraine attacks.
Chocolates and Cocoa Content
Chocolates, including dark chocolate, are often recommended during stress, mood swings, or hormonal changes. While some individuals may feel temporary emotional relief after consuming dark chocolate, chocolates are officially recognized as migraine stimulants.
Cocoa, the primary component of chocolate, directly affects pain pathways in the brain and can trigger migraine attacks. Regular chocolates also contain dairy ingredients, further increasing their stimulating potential. Therefore, both dark chocolates and milk-based chocolates should be avoided by individuals suffering from migraine.
Preservatives and Processed Foods
Preservatives are widely used in modern ready-to-eat and packaged foods. Although there is no single preservative responsible for migraine, foods containing preservatives often act as strong triggers. If a person notices that migraine symptoms worsen after consuming a particular packaged or processed food, it indicates sensitivity to the preservatives or additives present in that product.
Preservatives are harmful to everyone, but for migraine sufferers, they act as powerful stimulants that aggravate pain and neurological sensitivity. Sauces, packaged snacks, instant foods, and processed meals are particularly problematic.
Importance of Dietary Discipline in Naturopathic Management

In naturopathy, dietary regulation is considered a cornerstone of migraine management. During the initial phase of treatment—typically the first 60 days—patients are strictly advised to eliminate outside food, ready-made sauces, and preserved foods from their diet.
Freshly prepared, home-cooked food is always recommended, as it supports digestion, reduces toxin load, and helps in balancing Pitta dosha. A clean, simple, and natural diet plays a vital role in calming the nervous system and preventing migraine recurrence.
Importance of Home-Cooked Diet and Meal Regularity in Migraine Management
Diet plays a vital role in the prevention and management of migraine, especially from a naturopathic perspective. One of the most important dietary principles for migraine patients is the consumption of freshly prepared, home-cooked food. Home-cooked meals are easy to digest, hygienically prepared, and free from harmful preservatives and additives. When an individual prepares food for themselves or their family, it carries a sense of care and positivity, which contributes to mental satisfaction and emotional well-being—both of which are essential in migraine management.
Fresh food not only nourishes the body but also provides a positive psychological effect. Eating self-prepared meals enhances awareness, improves digestion, and supports the healing process. Therefore, ready-to-eat and packaged foods should be strictly avoided in migraine patients.
Avoidance of Ready-to-Eat and Packaged Foods
Even foods that are generally considered healthy, such as soups, can become problematic if consumed in packaged or instant forms. Although soups are often recommended to improve appetite and gut health, they must be prepared at home using fresh ingredients only. Packaged soup mixes contain preservatives, excess sodium, artificial flavors, and additives that can act as migraine triggers.
For migraine patients, every component of the diet should be natural, freshly prepared, and free from chemicals. This dietary discipline helps in reducing toxin load and calming the nervous system.
Artificial Sweeteners as Migraine Stimulants
Migraine is commonly observed in individuals suffering from diabetes and heart-related conditions, often appearing at an early age. One of the reasons behind this association is prolonged exposure to high blood sugar levels and the frequent use of artificial sweeteners.
Although white sugar is not recommended for health reasons, the continuous use of artificial sweeteners such as sugar-free tablets, drops, or powders is equally harmful—especially for migraine sufferers. These sweeteners are chemically synthesized and can disturb neurological balance, acting as strong stimulants for migraine.
Many people mistakenly believe that sugar-free products are safe, but from a naturopathic point of view, artificial sweeteners are completely contraindicated in migraine patients.
Natural Alternatives to Artificial Sweeteners
For individuals seeking safer alternatives, natural sweeteners are a better option when used in moderation. Jaggery is a natural sweetener that provides minerals and is easier for the body to process compared to refined sugar. Spirulina is another natural option that can help balance blood sugar levels while providing nutritional support.
Today, several natural alternatives are available, and selecting them wisely can help manage both blood sugar levels and migraine symptoms. However, artificial sweeteners should be completely avoided, particularly by individuals with migraine tendencies.
Understanding Triggers: Individual Variations
Migraine triggers vary significantly from person to person. What may be well tolerated by one individual could trigger severe migraine in another. This variability is the reason why migraine triggers are often represented with open-ended lists rather than fixed rules.
In clinical practice, it is commonly observed that some patients may tolerate certain foods like cheese, while others experience severe migraine after consuming them. Therefore, identifying personal triggers through observation and dietary awareness is essential for effective migraine management.
Skipping Meals: A Common and Dangerous Trigger
One of the most common and overlooked migraine triggers is skipping meals. Many individuals skip meals intentionally for weight loss or digestive improvement. However, skipping meals does more harm than good, especially for migraine patients.
Skipping meals not only increases the risk of migraine attacks but also contributes to nutritional deficiencies and metabolic imbalance. Instead of skipping meals, individuals should focus on modifying meal composition, such as choosing fiber-rich, nutrient-dense, and light foods.
Skipping grains may be acceptable for some individuals, but skipping entire meals is never advisable—particularly in migraine, digestive disorders, or chronic conditions.
Role of Digestive Fire (Agni) in Migraine
According to Ayurveda, the digestive fire, or Agni, plays a central role in maintaining health. Agni requires regular nourishment to remain balanced. When meals are skipped, Agni becomes disturbed, leading to symptoms such as dizziness, headache, heaviness in the forehead, and mental fatigue.
Many people notice that after long hours without food, they experience drowsiness, mild headache, or pressure around the forehead. This occurs because the body lacks the necessary glucose, nutrients, and energy required to maintain normal brain and nervous system function.
Food provides essential nutrients such as fibers, fats, glucose, vitamins, and minerals, which support all organs and systems in the body. When these nutrients are withheld, the imbalance affects multiple systems and ultimately triggers migraine episodes.
Role of Intense Physical Activity, Sensory Triggers, and Environmental Stimuli in Migraine
Lifestyle habits play a crucial role in triggering or preventing migraine episodes. Among these habits, intense physical activity and excessive sensory exposure are commonly overlooked yet powerful triggers. While exercise is essential for overall health, improper intensity, lack of guidance, and sudden overexertion can aggravate migraine symptoms rather than relieve them.
Intense Workouts and Migraine Aggravation
Many individuals approach weight loss with an extreme mindset, especially those who struggle to control food cravings. Instead of modifying diet habits gradually, they often compensate by engaging in excessive or intense workouts to burn extra calories. However, every body type has its own limitations, and physical activity must be aligned with individual capacity.
Workout routines should always begin gradually, especially for beginners. Intensity, duration, and speed should be increased slowly over time, ideally after several months of consistent practice. Sudden, high-intensity exercise—particularly with the goal of rapid weight loss—can be harmful to overall health and acts as a strong migraine trigger.
This risk is especially evident in gym-based workouts, where individuals may be encouraged to push beyond their physical limits. Without proper guidance or awareness of personal thresholds, intense workouts can lead to exhaustion, dehydration, hormonal imbalance, and neurological stress, all of which contribute to migraine attacks. Therefore, migraine patients are strongly advised to avoid intense workouts, particularly high-intensity gym routines, and instead follow moderate, well-guided physical activity plans.
Importance of Moderation and Personalization in Exercise
Exercise should support healing, not strain the body. For migraine sufferers, low to moderate intensity activities such as walking, gentle stretching, yoga, and controlled breathing exercises are more beneficial. These forms of movement help improve circulation, digestion, and mental balance without overstimulating the nervous system.
Personalized exercise plans that respect the body’s limits are essential, as overexertion can worsen migraine frequency and severity.
Strong Smells as Sensory Triggers
Strong odors are among the most common sensory triggers for migraine. Many individuals are sensitive or allergic to certain smells, and for migraine patients, exposure to strong fragrances can immediately provoke headache or pain.
For this reason, migraine sufferers are advised to avoid perfumes, deodorants, and heavily fragranced personal care products. Soaps, face washes, cosmetics, and household products containing artificial fragrances can also act as triggers and should be minimized or avoided.
Kitchen Odors and Occupational Exposure
In some cases, strong cooking odors can also trigger migraine episodes, particularly in individuals who spend long hours in the kitchen. The continuous inhalation of strong food aromas or spices may overstimulate the olfactory nerves, leading to headache or discomfort. This sensitivity varies from person to person but remains a significant trigger for many migraine patients.
Because smell is directly connected to breathing, repeated inhalation allows these sensory stimuli to affect both the lungs and the brain rapidly. This constant stimulation can disturb neurological balance and trigger migraine pain.
Preventive Measures for Smell Sensitivity
Migraine patients who are sensitive to odors are advised to take preventive measures, especially during travel or in unavoidable environments. Wearing a mask can help reduce exposure to triggering smells and provide a simple yet effective layer of protection.
Light Sensitivity and Flashlight Exposure
Excessive exposure to bright lights or flashing lights is another major migraine trigger. Many migraine patients experience sudden headache or pain after prolonged exposure to strong artificial lighting. This is particularly common during night travel, where continuous exposure to vehicle headlights and flashing lights can overstimulate the visual system.
Prolonged night driving or staying under intense lighting conditions can lead to visual strain, neurological fatigue, and migraine onset. Therefore, migraine sufferers should limit exposure to harsh lighting whenever possible and take regular breaks to rest their eyes.
Hormonal, Metabolic, Environmental, and Lifestyle Triggers in Migraine
Migraine is not caused by a single factor; rather, it is triggered by a combination of internal imbalances and external influences. Many individuals experience headache or migraine episodes after specific activities or exposures, and identifying these triggers is essential for effective prevention and management.
Travel-Related Triggers and Light Exposure
Many people report the onset of headache or migraine after long journeys. One of the primary reasons for this is continuous exposure to bright headlights, flashlights, and artificial lighting, especially during night travel. Prolonged visual strain overstimulates the nervous system and can trigger migraine attacks. This sensitivity to light is a well-recognized trigger and is commonly experienced by migraine patients during or after travel.
Hormonal Changes as a Major Trigger
Hormonal fluctuations are among the most common and powerful migraine triggers, particularly in women. Migraine episodes are frequently observed during menstrual cycles, where headaches may appear episodically rather than as a chronic condition. These headaches are directly related to hormonal secretions and fluctuations within the body.
Conditions such as PCOS, PCOD, and thyroid disorders further increase the risk of migraine due to hormonal imbalance. Women suffering from these conditions often report more frequent or severe migraine episodes. Any form of hormonal disturbance—natural or pathological—can significantly trigger migraine symptoms.
Dehydration and Fluid Imbalance
Dehydration is a serious health issue and, in some cases, can be life-threatening. For migraine patients, dehydration is one of the most common and preventable triggers. Maintaining adequate fluid intake is essential, even if food intake is reduced temporarily.
The human body consists of more than 70% water, and maintaining electrolyte balance is critical for proper neurological function. Migraine patients should ensure regular consumption of fluids such as plain water, lemon water, amla juice, fruit juices, vegetable juices, green juices, soups, or any easily digestible fluid that suits their body. Proper hydration helps stabilize the nervous system and prevents headache onset.
Hypoglycemia and Blood Sugar Fluctuations
Low blood sugar levels, or hypoglycemia, are another significant trigger for migraine, especially among diabetic patients. Hypoglycemic episodes often occur due to fluctuations in blood sugar levels or changes in medication dosage. Sudden drops in glucose levels affect brain function and can initiate migraine attacks. Maintaining stable blood sugar through timely meals and appropriate dietary choices is essential for migraine prevention.
Stress: A Universal Migraine Trigger
Stress is widely recognized as a root cause of many health conditions, including migraine. Even individuals without migraine experience fatigue, low energy, poor concentration, sleep disturbances, and emotional imbalance during periods of stress. For migraine patients, stress acts as a powerful trigger that intensifies both the frequency and severity of attacks.
It is important to acknowledge that complete freedom from stress is unrealistic. Every individual experiences stress; the key lies in how it is managed. Stress can be perceived negatively or transformed into a motivating or creative force. Effective stress management requires conscious effort, emotional balance, and the ability to divert the mind through relaxation techniques, hobbies, or mindfulness practices.
Climatic and Seasonal Changes
Environmental and climatic changes significantly influence migraine patterns. High temperatures during summer often lead to increased migraine episodes due to heat, dehydration, and Pitta aggravation. Similarly, winter season aggravates Kapha and Vata doshas, making individuals with Kapha-related tendencies more susceptible to migraine attacks.
Sudden changes in weather, humidity, or temperature disturb the body’s internal balance and act as natural migraine triggers. Seasonal sensitivity varies from person to person, depending on individual constitution and dosha dominance.
Irregular Sleeping Patterns and Shift Work

Irregular sleep schedules are a major contributing factor to migraine. Individuals working night shifts, rotating shifts, or long working hours—such as those in research laboratories, healthcare, or technical fields—are particularly vulnerable. Disrupted circadian rhythm affects hormonal balance, mental alertness, and nervous system stability, all of which can trigger migraine episodes.
Lack of adequate rest, prolonged standing, and irregular sleep-wake cycles strain the body and brain, increasing susceptibility to headache and migraine.
Irregular Sleep Patterns, Biological Clock Disruption, and Screen Time as Modern Migraine Triggers
In today’s fast-paced lifestyle, irregular work schedules have become increasingly common. Individuals working in factories, multinational companies, call centers, research organizations, and corporate sectors often have to adjust their routines according to rotating shifts or international time zones. While this work structure may be professionally necessary, it poses serious health challenges—particularly for individuals suffering from migraine.
Shift Work and Irregular Sleeping Schedules
Shift work is one of the strongest modern triggers for migraine. People who work night shifts or rotating shifts are unable to maintain a fixed sleep–wake cycle. This irregular sleeping pattern disrupts the body’s natural rhythm and places immense stress on the nervous and hormonal systems.
The human body functions according to a biological clock, also known as the circadian rhythm. This internal clock regulates sleep, digestion, hormone secretion, metabolism, and organ repair. For optimal health, daily activities should align as closely as possible with this natural rhythm. When individuals consistently ignore or override this internal clock, health imbalances begin to develop, and migraine is one of the earliest warning signs.
Organ Function and Night-Time Physiology
Both modern science and Ayurveda acknowledge that different organs perform specific functions at specific times during the night. For example, after an early dinner, it takes approximately four to five hours for food to be completely digested. Once digestion is complete, internal repair and detoxification processes begin.
Research and traditional health sciences indicate that:
- The liver becomes most active between 11:00 PM and 3:00 AM, performing detoxification and metabolic regulation.
- After this phase, the digestive and restorative systems continue their work to prepare the body for the next day.
When a person is asleep during these hours, organs are able to function smoothly and efficiently. However, if an individual remains awake, eats food, or engages in physical or mental activity during this period, the organs are forced to work under strain. This added burden disrupts metabolic balance and leads to toxin accumulation, which can directly trigger migraine episodes.
The liver, often referred to as the body’s largest chemical factory, plays a crucial role in hormone regulation, detoxification, and energy metabolism. Any disturbance in liver function—especially due to irregular sleep—can result in biochemical imbalances that contribute to migraine onset and severity.
Screen Time: A New-Age Migraine Trigger
Over the past 8 to 10 years, excessive screen time has emerged as a significant migraine trigger. With the rise of digital education, remote work, and online communication, prolonged screen exposure has become unavoidable for many professionals.
Corporate employees often spend 10 to 12 hours continuously in front of screens, focusing on computers, laptops, or mobile devices with minimal breaks. This constant visual strain overstimulates the nervous system and leads to eye fatigue, mental exhaustion, and migraine attacks.
While screen use may be unavoidable for professional reasons, unnecessary and prolonged screen exposure without breaks is increasingly common among youngsters, homemakers, and the general population. Sitting continuously in front of a screen for more than 90 minutes without a break can significantly increase the risk of headache and migraine.
Impact of Continuous Screen Exposure
Excessive screen time affects migraine patients in multiple ways:
- Continuous exposure to artificial light strains the eyes and optic nerves.
- Mental overuse increases neurological fatigue.
- Blue light disrupts melatonin secretion, further disturbing sleep cycles.
- Poor posture during screen use increases neck and shoulder tension, which can radiate pain to the head.
These combined effects make prolonged screen exposure one of the most important lifestyle-related migraine triggers in modern society.
Risk Factors and Common Symptoms of Migraine
Migraine is influenced not only by immediate triggers and stimulants but also by certain risk factors that increase an individual’s susceptibility over time. Some people may not experience migraine symptoms in the early stages of life, yet they remain at higher risk of developing migraine as they grow older. Understanding these risk factors allows early preventive measures and significantly reduces the likelihood of future migraine episodes.
Family History as a Major Risk Factor
One of the most significant risk factors for migraine is family history. Nearly 90% of migraine cases are hereditary, meaning individuals with a family history of migraine are much more prone to developing the condition. If parents, siblings, or even ancestors across several generations have suffered from migraine, the risk is considerably higher.
However, having a family history does not mean that migraine is inevitable. Awareness plays a crucial role in prevention. Individuals who know they carry a genetic predisposition can adopt preventive lifestyle measures early in life. By avoiding known triggers and stimulants, maintaining healthy routines, and following naturopathic principles, it is possible to prevent migraine onset altogether. With proper precautions, there is also a strong possibility of stopping the continuation of migraine tendencies from one generation to the next.
Importance of Preventive Awareness
Migraine is not a condition that must occur simply because of heredity. Genetic tendency only creates susceptibility, not certainty. Early identification of risk factors and conscious lifestyle modifications can significantly reduce or even eliminate migraine risk. Preventive care is especially effective when started before symptoms appear.
Common Symptoms of Migraine
Migraine presents with a characteristic set of symptoms that differentiate it from ordinary headaches. The most prominent symptom is headache pain, but its location and nature are distinct.
One-Sided or Frontal-Temporal Headache
Migraine pain typically occurs on one side of the head or in the frontal-temporal (front temple) region. This unilateral pain is a hallmark of migraine. In Ayurveda, migraine is referred to as “Ardhavabhedaka”, meaning pain affecting half of the head. This term accurately reflects the classical presentation of migraine and highlights its long-standing recognition in traditional medicine.
Neck Pain and Stiffness
Many migraine patients also experience pain or stiffness in the neck region. This occurs due to muscular tension and neurological involvement extending from the head to the neck. The pain may radiate from the frontal area to the neck or shoulder region, intensifying discomfort.
Loss of Appetite

Loss of appetite is a very common symptom during migraine episodes. When the body experiences intense or prolonged pain, its focus shifts toward managing that pain, leading to reduced digestive activity. Migraine pain often lasts longer than common headaches and does not resolve immediately, even with medication.
As a result, digestive processes slow down, leading to decreased hunger and sometimes nausea. This loss of appetite is a natural physiological response during migraine attacks.
Redness of Eyes
Red or bloodshot eyes are another symptom observed during migraine episodes. Continuous and unbearable pain causes vascular and neurological stress, leading to eye redness and sensitivity. This symptom often accompanies prolonged or severe migraine attacks.
Risk Factors, Symptoms, and Diagnosis of Migraine
Migraine is a complex neurological condition influenced by multiple triggers, stimulants, and risk factors. While many people may be exposed to these risk factors, not everyone experiences migraine immediately. However, with increasing age or prolonged exposure, the likelihood of developing migraine increases significantly. Understanding these risk factors, symptoms, and diagnostic criteria plays a crucial role in early prevention and effective management.
Major Risk Factors of Migraine
Among all known risk factors, family history stands out as the most significant. Approximately 90% of migraine cases are hereditary in nature. Individuals whose parents, siblings, or even ancestors over four to five generations have suffered from migraine are at a much higher risk. This genetic predisposition does not guarantee that a person will definitely suffer from migraine, but it does indicate a strong possibility.
Awareness is the key preventive measure in such cases. If an individual knows that migraine runs in their family, taking early precautions—such as avoiding known triggers and maintaining a disciplined lifestyle—can significantly reduce the chances of developing migraine. In fact, with conscious preventive efforts, it is possible to stop the continuation of migraine from one’s generation onward.
Common Symptoms of Migraine
The most well-known symptom of migraine is headache, but it has specific characteristics that differentiate it from common headaches. Migraine pain typically occurs in the front-temporal region or is one-sided, affecting either the right or left half of the head. This is why migraine is referred to as “Ardhavbhedaka” in Ayurvedic texts, meaning pain affecting half of the head.
Another frequent symptom is neck pain, which occurs due to the involvement of surrounding nerves and muscles connected to the frontal and cervical regions. Loss of appetite is also commonly observed. During a migraine attack, the body’s focus shifts entirely toward managing pain, slowing down the digestive system and naturally reducing hunger.
Redness of the eyes may appear in some individuals. Continuous and intense pain can cause changes in blood flow around the eye region, leading to dryness, irritation, or redness. Although this symptom does not occur in every case, it is commonly associated with severe migraine episodes.
Palpitations are another possible symptom. Prolonged pain often leads to irritation, discomfort, and heightened anxiety levels. This mental and physical stress can temporarily increase heart rate, resulting in palpitations.
It is important to note that symptoms vary from person to person. Some individuals may experience only one or two symptoms, while others may experience several simultaneously. When such symptoms persist for a long duration and occur at regular intervals, it becomes essential to seek medical consultation to confirm whether the condition is migraine or related to other internal imbalances.
Understanding Migraine Diagnosis
Unfortunately, there is no single specific laboratory test to diagnose migraine. Unlike conditions such as diabetes or cancer—where definitive blood tests and markers are available—migraine diagnosis relies primarily on clinical evaluation.
Doctors consider multiple factors such as:
- Family history
- Frequency and duration of headache episodes
- Associated symptoms
- Age and gender
- Presence of other health conditions or deficiencies
Clinical history and family history remain the most important tools in diagnosing migraine, irrespective of the medical system or pathy being followed.
According to standard diagnostic criteria, a person is usually considered a migraine patient if they have experienced at least five headache attacks, each lasting between 5 to 72 hours, along with characteristic symptoms.
Classification Based on Diagnostic Criteria
Migraine is further classified based on specific symptom patterns. One key category includes individuals who experience unilateral headaches, meaning pain restricted to one side of the head. Another criterion is moderate to severe intensity of pain, which often starts mildly and gradually increases in severity.
Migraine pain commonly worsens with routine physical activity, leading individuals to avoid daily tasks and responsibilities. This avoidance is not intentional but a natural response to severe discomfort, irritation, and inability to concentrate.
Diagnostic Criteria and Management Approach for Migraine
Migraine is diagnosed primarily on the basis of clinical symptoms rather than a single definitive laboratory test. Certain characteristic symptom patterns help physicians distinguish migraine from a routine or tension-type headache.
Symptom-Based Diagnostic Criteria
If a patient experiences any two symptoms from a specific symptom group, the condition is highly suggestive of migraine. Common associated symptoms include nausea and vomiting, which frequently accompany migraine attacks. Many patients also experience photophobia (sensitivity or fear of light) and phonophobia (sensitivity or fear of sound).
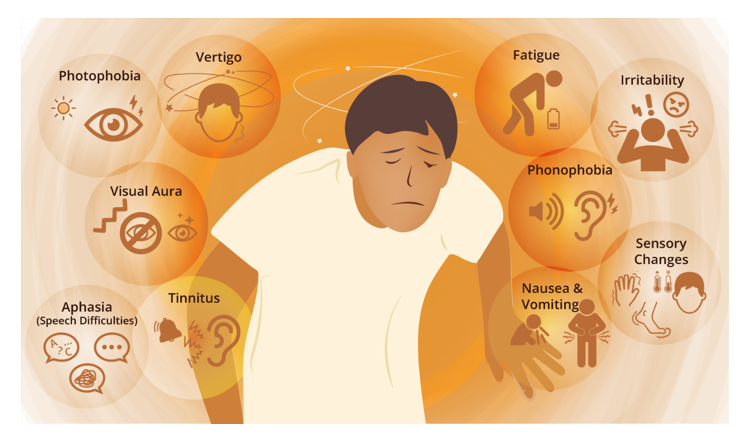
Exposure to bright or flashing lights—such as high-voltage lights, screen glare, or camera flash—can immediately trigger or worsen a migraine episode. Similarly, loud noises from social gatherings, parties, public functions, microphones, or even mobile phone ringtones can intensify pain. This sound sensitivity is clinically referred to as phonophobia.
In some cases, patients may also experience fever and shivering along with headache. When any two symptoms from these diagnostic criteria are present along with characteristic headache patterns, the likelihood of migraine becomes very high.
These symptom combinations act as important “clinical checkpoints” that help doctors differentiate migraine from common headaches. Based on this structured evaluation, physicians can confidently determine whether a patient is suffering from migraine.
Role of Clinical Evaluation and Investigations
Once a detailed clinical and family history is taken, and the symptoms strongly indicate migraine, doctors may recommend further investigations. Since migraine is a chronic neurological condition, advanced diagnostic tools are sometimes used to rule out other neurological disorders.
Common investigations include MRI or CT scans of the head, which help exclude structural abnormalities or serious neurological conditions. Blood tests such as ESR (Erythrocyte Sedimentation Rate) and CRP (C-Reactive Protein) are also advised in some cases.
ESR is a marker of inflammation or infection. Normally, ESR values range between 0 to 20 mm/hour. Significantly elevated levels—such as values above 50 or 100—may indicate underlying infection or inflammatory conditions that could contribute to headache severity. CRP serves a similar purpose; elevated levels suggest active inflammation in the body, which may aggravate migraine symptoms.
By correlating clinical findings with laboratory and imaging results, physicians can arrive at an accurate diagnosis and rule out secondary causes of headache.
Treatment Approach for Migraine
Once migraine is diagnosed, treatment is usually focused on managing acute attacks and preventing recurrence. For immediate relief, doctors often prescribe over-the-counter (OTC) painkillers, selected according to the patient’s age, severity of symptoms, and overall health status. In recent years, certain medical devices have also been introduced to help reduce migraine pain and frequency.
However, medication alone is not sufficient, especially in cases of chronic migraine. Chronic migraine patients often experience severe, long-lasting pain that may continue for two to three days, sometimes without adequate relief even after taking painkillers.
Importance of Behavioral Therapy and Lifestyle Modification
Behavioral therapy plays a crucial role in managing chronic migraine. Prolonged pain can lead to irritability, anxiety, hypersensitivity, and emotional stress, which further worsen migraine episodes. Behavioral therapy focuses on modifying daily habits and responses to stress.
Lifestyle changes form the foundation of long-term migraine management. These include:
- Improving food habits
- Maintaining a disciplined daily schedule
- Ensuring adequate and regular sleep
- Managing stress effectively
- Adopting healthy coping mechanisms
Transforming daily routines, eating patterns, and overall lifestyle significantly reduces the frequency, intensity, and duration of migraine attacks. A combined approach of medication, behavioral therapy, and lifestyle modification not only helps control migraine episodes but also improves overall quality of life.
Naturopathic and Ayurvedic Approach to Migraine Management
From a naturopathic perspective, migraine is not merely a neurological disorder but a manifestation of deeper internal imbalances. Whether the migraine is episodic or chronic, naturopathy focuses on identifying and correcting the root cause rather than suppressing symptoms. As explained earlier, the primary underlying factor in migraine, according to naturopathy and Ayurveda, is the aggravation of Pitta dosha.
Role of Pitta Dosha in Migraine
Pitta represents heat, metabolism, and transformation within the body. There are approximately 80 different functional expressions of Pitta operating in various organs and systems. However, not every individual with aggravated Pitta develops migraine. Some experience burning sensations, excessive sweating, internal heat, acidity, nausea, or sour vomiting. Others notice a persistent bitter taste in the mouth, excessive salivation, or a thick white coating on the tongue.
When specific forms of Pitta become imbalanced—especially those related to the nervous system, liver, digestion, and blood—it can lead to migraine. Therefore, the first and most crucial step in naturopathic migraine treatment is to balance all three doshas: Vata, Pitta, and Kapha. Only after restoring this balance can effective detoxification and healing begin.
Importance of Detoxification and Dosha Balance
Detoxification plays a central role in migraine management. According to naturopathy, the body must be cleansed thoroughly—from superficial tissues to deep cellular levels. Blood purification and removal of accumulated toxins are essential. Detoxification helps normalize aggravated Pitta, stabilizes the nervous system, and improves circulation and digestion.
Balancing the three doshas along with systematic detoxification creates a strong foundation for long-term migraine relief.
Mud Therapy (Earth Element Therapy)

Mud therapy is derived from the earth element and is highly effective in cooling aggravated Pitta. Natural deep-sea or mineral-rich mud possesses cooling, absorbent, and detoxifying properties. In migraine management, mud is applied to the head and feet simultaneously.
This application helps draw out excess heat from the body, relaxes the nervous system, and improves circulation. The cooling nature of mud soothes inflammation and provides immediate calming effects.
Hot and Cold Foot Bath Therapy
Hot and cold foot baths are an effective naturopathic technique to regulate nerve stimulation and circulation. This therapy involves alternating foot immersion in warm water and normal-temperature cold water.
Typically, the therapy lasts 20 to 30 minutes, with 10–15 minutes in warm water followed by 10–15 minutes in cold water. The warm water promotes vasodilation (expansion of blood vessels), while the cold water causes vasoconstriction (contraction). This alternating stimulation relaxes overactive nerves, reduces internal congestion, and relieves migraine triggers.
Magnet Therapy and Acupressure Stimulation
Magnet therapy, also referred to as Nadi Chikitsa in naturopathy, does not require electrical or mechanical devices. Specially prepared stones or materials are magnetized naturally over time and used therapeutically.
A magnetized stone or drift is rubbed gently on the feet using a bronze vessel (bronze vati) with 8–10 drops of cow ghee or medicated ghee. This is done for 5 to 10 minutes daily before bedtime.
The feet contain over 276 acupressure points, many of which are connected to the brain and nervous system. Instead of targeting specific points, whole-foot stimulation ensures balanced activation, helping reduce headache intensity and frequency.
Nasya Therapy (Nasal Oil Application)
Nasya therapy is a powerful Ayurvedic treatment for disorders above the neck, including migraine. Medicated oils such as Anu Taila, Goghrita (cow ghee), or other Ayurvedic oils are commonly used.
Every night before sleeping, 3–4 drops of the oil are instilled into each nostril. This practice nourishes the nasal passages, calms the nervous system, improves brain circulation, and reduces migraine recurrence.
Pranayama (Air Therapy)
Pranayama, or regulated breathing, plays a vital role in neurological health. Oxygen therapy through controlled breathing enhances brain function and reduces stress-induced migraine triggers.
Three specific pranayama techniques are highly recommended:
- Om Pranayama
- Bhramari Pranayama
- Anulom Vilom
Each should be practiced for 10 cycles daily. For individuals who feel discomfort practicing with closed eyes, pranayama can be safely performed with eyes open. Comfort and consistency are more important than strict rules.
Lifestyle and Dietary Modifications
Lifestyle correction is fundamental in migraine management. Foods that aggravate Pitta—such as excessively spicy, oily, fried, fermented, or acidic foods—must be avoided. Instead, a diet rich in fiber, fluids, and alkaline foods should be adopted.
An ideal dietary pattern includes:
- 60% raw food (fruits, salads, sprouts)
- 40% cooked food
- Seasonal and regional fruits once daily
For individuals weighing around 50–55 kg, daily fruit intake should be 250–300 grams, preferably consumed in the morning as part of breakfast. Grains and cooked foods should be avoided during breakfast. Starting the day with high-fiber, alkaline foods significantly reduces headache severity.
Adequate hydration, regular meal timing, and early dinners are essential. Sleep should ideally follow the natural rhythm, from 10 PM to 6 AM, allowing proper organ detoxification.
Discipline, Routine, and Sleep Hygiene
A disciplined daily routine is critical for migraine sufferers. Irregular schedules disturb the biological clock and worsen symptoms. Punctuality, consistency in meals, sleep, and work habits help stabilize the nervous system and reduce migraine episodes.
Detoxifying Herbs for Migraine Relief
Certain herbs are especially effective in reducing Pitta, detoxifying the body, and improving gut–brain health. Based on long-term clinical experience, the most effective detox herbs include:
- Fresh Aloe Vera – A powerful blood purifier and digestive cleanser
- Dalbergia (Indian Kino) – One of the most alkaline substances, second only to wheatgrass
- Amruda (Guava) – Boosts immunity, balances all three doshas, and improves digestion
These herbs support detoxification, regulate Pitta, and strengthen the gut–brain connection.
Supportive Ayurvedic Formulation for High Pitta
For individuals with high Pitta, additional herbs can be included:
- Amlaki
- Suta Shankhar
- Avipattikar Churna
- Yashtimadhu
- Shatavari
These herbs can be mixed in equal proportions to prepare a churna (powder). One spoonful of this mixture should be taken daily after meals with ghee or plain water. This formulation is safe and beneficial even for individuals with other health conditions.
Home Remedies and Ayurvedic Supportive Therapies for Migraine Relief
Along with detoxification, lifestyle correction, and internal herbal support, certain simple Ayurvedic home remedies play a very effective role in managing migraine. These remedies are safe, natural, easily available, and can be used regularly without side effects when applied correctly.
Role of Saffron in Migraine Management
Classical Ayurvedic literature mentions saffron (Kesar) as a powerful herb that helps balance the three doshas, particularly Pitta and Vata. Saffron has a cooling and calming effect on the nervous system. It is known to:
- Support neurological health
- Improve vision
- Reduce headache intensity
- Calm mental agitation and anxiety
Because of its cooling and dosha-balancing properties, saffron is beneficial in migraine, especially when symptoms are aggravated by heat, stress, or emotional imbalance.
Nasya Therapy with Ghee
As discussed earlier, Nasya therapy using clarified butter (cow ghee or Goghrita) is highly effective in migraine. Ghee acts as a Vata-Pitta shamak, meaning it pacifies both Vata and Pitta doshas.
Regular application of 3–4 drops of warm ghee into each nostril before bedtime nourishes the nasal passages, calms the nervous system, improves circulation to the brain, and provides relief from chronic headaches and migraine episodes.
Facial and Neck Massage (Abhyanga)
Massage therapy (Abhyanga) using cooling oils is another effective supportive treatment. Oils such as:
- Sesame oil
- Coconut oil
can be gently massaged over the frontal region, temple area, face, and neck, particularly where pain is most intense. This therapy relaxes tight muscles, improves blood circulation, reduces stiffness, and provides immediate comfort during migraine attacks.
Potli Therapy with Carom Seeds (Ajwain Potli)
One of the most effective and simple home therapies is Ajwain Potli therapy.
Method:
- Take 1 tablespoon of carom seeds (Ajwain)
- Wrap them in a clean white cotton cloth to form a small potli
- Warm the potli lightly on a tawa (do not overheat)
- Once comfortably warm, gently rub or massage the potli over:
- Forehead
- Temple region
- Neck or affected area
This therapy provides quick pain relief, improves circulation, and reduces nerve irritation. It should be warm, not hot, to avoid discomfort.
Black Raisin Herbal Drink for Chronic Migraine
A highly effective internal home remedy for chronic migraine involves black raisins, coriander seeds, fennel seeds, and black salt.
Preparation Method:
- Soak 15–20 black raisins in water overnight
- In the morning, boil the soaked water
- Add:
- 1 teaspoon whole coriander seeds
- 1 teaspoon fennel seeds
- A pinch of black salt
- Boil for 5 minutes until the quantity reduces to half
- Strain and consume warm on an empty stomach
This drink helps cleanse the system, balances Pitta, improves digestion, and significantly reduces migraine frequency when taken regularly.
Cooling External Applications
Certain topical applications are helpful during migraine attacks due to their cooling and soothing properties:
- Sandalwood paste
- Fresh aloe vera gel
Applying these over the forehead and temple area helps reduce irritation, inflammation, heat, and anxiety associated with migraine. These applications also provide mental calmness during acute episodes.
Importance of Managing Constipation
Constipation is a major contributing factor in migraine. If bowel movements are not regular, no diet, medicine, or therapy will give lasting relief. Proper elimination is essential for dosha balance.
To manage constipation:
- Use mild herbal cleansers like Triphala and Yashtimadhu (Mulethi)
- Increase fiber and fluid intake
- Maintain regular meal and sleep timings
Detoxification must always begin with bowel regulation for successful migraine management.
Herbal Powder Combination for Pitta Balance
For internal use, the following herbs can be mixed in equal proportion (powder form):
- Suta Shankhar
- Avipattikar Churna
- Yashtimadhu (Mulethi)
- Shatavari
Dosage:
Take 1 teaspoon daily after meals with ghee or plain water.
This formulation helps reduce acidity, balance Pitta, improve digestion, and calm the nervous system. It is safe for adults and can be adjusted for children under guidance.
Safety and Use in Children
All remedies mentioned—Ajwain potli, ghee nasya, raisin water, massage oils—are safe for children when used gently and in appropriate quantities. Since these remedies are derived from kitchen ingredients and natural substances, they can be used without fear of side effects.
Seasonal Considerations
Migraine symptoms may worsen in certain seasons, especially winter, due to Vata aggravation. In such cases, oil therapies, ghee nasya, and warm applications become even more beneficial.
Conclusion
Migraine is a complex neurological disorder influenced by a combination of genetic, lifestyle, dietary, hormonal, and environmental factors. While stimulants such as alcohol, caffeine, processed foods, chocolates, artificial sweeteners, and strong fragrances can trigger attacks, lifestyle habits like irregular sleep, intense workouts, prolonged screen time, and stress further exacerbate the condition. Hormonal fluctuations, dehydration, climatic changes, and shifts in biological rhythm also play a significant role in aggravating migraine episodes.
The symptoms of migraine vary but commonly include unilateral headache, neck pain, nausea, vomiting, photophobia, phonophobia, red eyes, palpitations, and loss of appetite. Diagnosis relies primarily on clinical and family history, with advanced tests like MRI, CT scans, and blood tests used to rule out other conditions. Recognizing early signs and patterns is essential for timely intervention.
Conventional treatment focuses on acute pain relief and preventive medications, often complemented by behavioral therapy. However, for long-term relief, a holistic and naturopathic approach proves highly effective. Naturopathy emphasizes balancing the doshas (especially Pitta), detoxifying the body, and restoring neurological harmony through mud therapy, hot and cold foot baths, magnet therapy, nasya, pranayama, and lifestyle modifications. Incorporating a fiber-rich, alkaline, seasonal diet, maintaining hydration, adhering to sleep schedules, and avoiding triggers form the foundation of preventive care.
Herbal remedies such as aloe vera, Dalbergia, amla, Shatavari, Yashtimadhu, and Avipattikar churna support digestion, immunity, and Pitta balance. Simple home therapies like carom seed potli massages, black raisin water with fennel and coriander, and topical applications of sandalwood or aloe vera provide immediate relief. Addressing gut health and constipation is essential to enhance the effectiveness of these therapies.
Ultimately, managing migraine requires a disciplined, holistic lifestyle combined with awareness of triggers, preventive care, and naturopathic interventions. By adopting a balanced routine, maintaining dietary and sleep discipline, and using herbal and home remedies, individuals can significantly reduce the frequency and severity of migraine attacks, leading to improved health, well-being, and quality of life.








